Reaching New Heights: Digitally Connecting the Fight Against Esophageal Cancer in East Africa
Dr. Gift Mulima (KCH), James Ndungu (Proximie), and Dr. Michael Mwachiro (Kenya) together in Malawi—building a regional vision for surgical training
In the heart of East Africa, a quiet revolution is taking place—one that blends surgical mentorship, cutting-edge digital innovation, and powerful cross-border collaboration to fight one of the region’s deadliest cancers: Esophageal Squamous Cell Carcinoma (ESCC).
This March, Kamuzu Central Medical Center (KCH) in Malawi became the first site in the country to deploy Proximie, a digital surgical collaboration software platform. This deployment is part of a visionary initiative by the African Esophageal Cancer Consortium (AfrECC) to scale critical esophageal cancer training and mentorship across the region.
Leading this bold charge is Dr. Michael Mwachiro, a renowned Kenyan surgeon, educator, chair of the COSECSA Education, Research and Scientific Committee and Vice President of the Surgical Society of Kenya. At KCH, he is joined by Dr. Gift Mulima, a Malawian general surgeon and endoscopist mentored by Mwachiro—now passing his knowledge forward to the next generation.
“Everyone is learning together to reach new heights of capacity.”
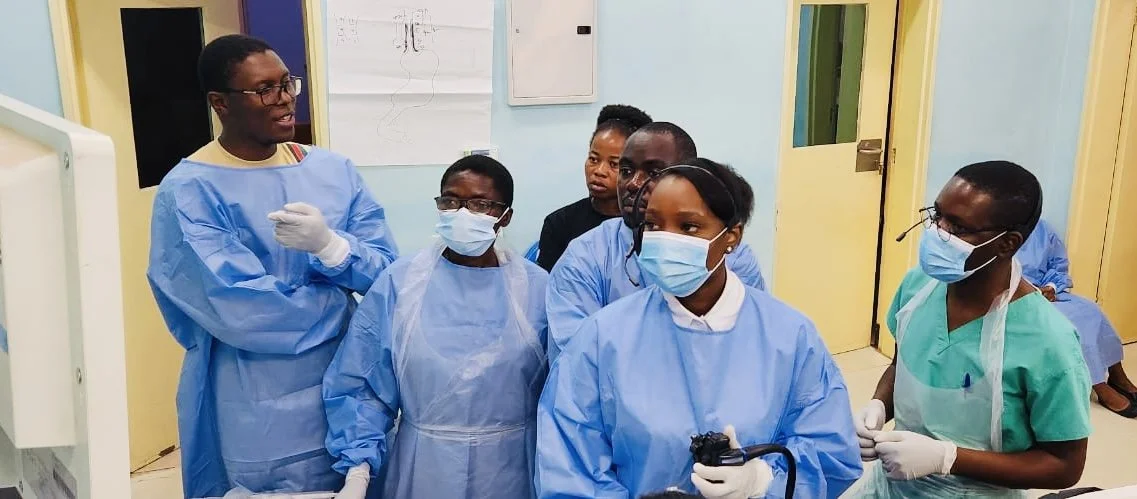
Mentorship in action: Dr. Mwachiro and Dr. Mulima guiding four Malawian surgeons through six hands-on cases a day in Lilongwe.
The Urgent Need: A Cancer Crisis in East Africa
Esophageal cancer, particularly ESCC, is an underrecognized public health crisis in Africa.
🌍 Africa recorded an estimated 30,000 new cases and 28,000 deaths from ESCC in 2022.
🚨 By 2045, projections rise to 65,000 cases and 62,000 deaths (Morgan et al., 2022).
🇲🇼 Malawi has the highest incidence rate in the world.
⏳ Over 90% of patients present with advanced disease, and survival rates remain below 5%.
Contributing risk factors identified by AfrECC research include:
High exposure to polycyclic aromatic hydrocarbons (PAHs) from indoor smoke (Mwachiro et al., 2016)
Drinking extremely hot beverages (Islami et al., 2009)
Poor oral health and nutritional deficiencies, including low selenium (Simba et al., 2023)
AfrECC—a growing network of 130+ scientists and clinicians across 19 countries—has taken the lead in early detection, risk mapping, and training programs. But to scale sustainably, they wanted a digital leap.
The Digital Leap: How Proximie is Transforming Training
Proximie is a secure, AWS cloud-based software that enables:
✅ Live surgical mentoring
✅ Asynchronous video reviews
✅ Augmented reality overlays
✅ Low-bandwidth functionality for remote, rural hospitals
Today at Kamuzu Central Hospital: Proximie is fully installed, the team is trained, and the first live sessions are underway
At KCH this week, Proximie—enabled by AWS—is digitally powering AfrECC’s esophageal stent placement training, part of a broader workshop series generously supported by Boston Scientific.
James from Proximie, Dr. Mwachiro with Kirk and Sylvie from Boston Scientific
Together, they will build a borderless digital surgical community where mentorship, continuous education, and peer collaboration are no longer constrained by geography.
“It’s not just technology—it’s apprenticeship without borders.”
Dr. Mwachiro, envisages a series of upcoming Proximie powered, AWS enabled hubs in Kenya, Ethiopia, Uganda and beyond to connect this growing AfrECC community together in a borderless manner. A 2023 review confirmed that post-operative video benchmarking and self-assessment tools significantly enhance learning and skill retention among surgical trainees (Morgan et al., 2022)—eventually, a key advantage of Proximie’s cloud-based case library.
On the Ground: A Week of Hands-On Healing and Training
From Monday to Friday this week, a dedicated surgical camp is running at KCH. Under the mentorship of Dr. Mwachiro and Dr. Mulima, four local surgeons are being trained, with a daily rhythm that includes:
An average of three esophageal palliative stents placed per day
An additional three urgent cases daily managing GI bleeds and esophageal varices—patients who had been waiting for this moment, this team
Many of the stenting patients over the past two days are elderly. The youngest today was just 46 years old. Each stent placed represents a profound shift in the patient's quality of life. For those too advanced for curative surgery, these palliative stents offer something equally powerful: the ability to swallow, to nourish, to be present in life again.
“Palliative care, in this context, is not the end—it’s a return to life.”
Prior to intervention, many patients couldn’t swallow their own saliva. Some were dangerously malnourished, isolated by their symptoms. A simple stent can restore dignity, nutrition, and connection—at home, at the table, with family and friends.
AfrECC’s partnership with Boston Scientific goes far beyond sponsorship. Together, they’re ensuring access to affordable stents and hands-on insertion training that can scale with local needs.
And the four surgeons being trained this week? They’re not just participating—they’re being woven into an ongoing mentorship loop with Dr. Mwachiro and other AfrECC experts through Proximie. The sessions on Proximie this week will also serve as exemplar case studies and digital learning tools, allowing trainees and future participants to revisit the content, reflect on key steps, and reinforce their learning over time.
Building the Workforce We Need
Sub-Saharan Africa faces one of the world’s most severe surgical workforce shortages, with fewer than 1 surgeon per 100,000 people in many areas. Globally, the WHO predicts a shortfall of 18 million health workers by 2030, many of whom are needed in surgical care.
Digital technologies like Proximie are no longer optional—they’re essential. They enable:
Task sharing and remote case support
Equitable access to advanced surgical education
Scalable, consistent mentorship in resource-limited settings
A landmark study by ReSurge International and Stanford University modeled the lifetime impact of surgical training. It revealed that one surgeon in a low-income country can treat 10,000 patients during their career. But if that same surgeon becomes a full-time trainer, the impact multiplies to over 400,000 lives through their trainees (Cai et al., 2024).
This “multiplier effect” makes the case for investing not just in surgery, but in surgical education as a tool for generational impact.
Making It Real: Proximie’s Implementation at KCH, Today and Tomorrow
This is not a story about a future plan—it’s a story about what’s already happening as we speak.
After months of careful co-design between AfrECC's local surgical champions, and Proximie, the platform has now been formally and fully implemented at Kamuzu Central Hospital (KCH) in Malawi.
✅ Cameras have been installed.
✅ Local surgeons and endoscopy teams have been trained.
✅ Live mentorship sessions are underway.
Proximie is now enabling synchronous mentorship during procedures, as well as asynchronous case review for reflection, benchmarking, and collaborative learning. Recordings are stored securely and integrated into the training ecosystem, ensuring continuity.
In the short term, KCH will use Proximie to:
Reinforce learning from the current workshop
Host follow-up mentoring sessions
Expand into general endoscopy and laparoscopic education
In the medium term, KCH becomes a digital anchor hub—joining a regional community of surgical practice across Kenya, Uganda, Ethiopia, and beyond.
This isn’t a pilot. This is a blueprint.
A Regional Success Story in the Making
Dr. Gift Mulima’s journey—from mentee to mentor in Malawi—is the embodiment of AfrECC’s vision: a sustainable, Africa-led ecosystem of mentorship, clinical capacity, and regional leadership.
As Proximie expands its footprint to 7 countries in East Africa, enabled by AWS, each new site adds a layer to a growing network of trust, shared learning, and resilience.
This is digital global health at its best: African-led, collaborative, and future-facing.
A new community of practice is already taking shape—one shared case, one connection, one confident surgeon at a time.
If you care about health equity, cancer outcomes, or surgical training—this is a movement to watch.
Let’s build it together.
🧾 References
Cai, L., Meyers, N. & Chang, J. (2024). Modeling the lifetime impact of reconstructive plastic surgery training: Implications for building capacity in global surgery. Plast Reconstr Surg Glob Open, 12:e5577. https://doi.org/10.1097/GOX.0000000000005577
Islami, F., Boffetta, P., Ren, J.S., Pedoeim, L., Khatib, D. & Schottenfeld, D. (2009). High-temperature beverages and esophageal cancer risk: a systematic review. Int J Cancer, 125(3), pp.491–524.
Morgan, E., Mwachiro, M., et al. (2022). Esophageal Cancer in Africa: Epidemiology, Risk Factors and Challenges. Gastroenterology.
Mwachiro, M., Parker, R., Chepkwony, R., Burgert, S. & White, R.E. (2016). Screening for esophageal dysplasia using Lugol’s chromoendoscopy in a high-incidence African population. Am J Gastroenterol.
Simba, P., Kaimila, J., Mwachiro, M., et al. (2023). Patient beliefs and ESCC risk factor assessment in East Africa. JCO Global Oncology.